Many parents, therapists and physicians would consider this boy’s function a therapeutic success. I do not!
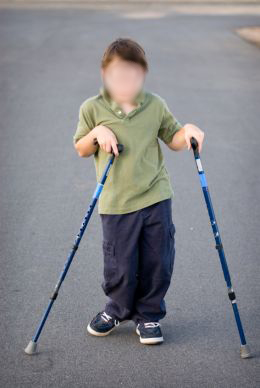
For children in GMFCS III to V, the long term studies have documented that there is an expected deterioration in function as they grow through puberty.1 Even though their brains continue to mature, allowing new function, their bodies develop new or worse distortions. When I look at this boy, I see the potenial for him to lose function.
Much of this can be prevented with age appropriate therapy and spasticity management. The child pictured above is doing well, but look at his hands. Hands held in flexion have a weak grasp as you can see by how he is holding his canes. Even in a child with a very functional hand, this type of wrist weakness leads to poor writing and typing speed that only really becomes evident in the teen years when the academic demands go up. This wrist position, in less functional hands, adds to the difficulty of learning any fine motor task. I suggest parents look back at photos of their child’s hand at earlier ages and see for themselves the slow, but steady loss of alignment and strength. Neuroplasticity and Hands: Doing The Right Thing, At The Right Time, and In The Right Order
Now look at his body and legs. He has increased tone, more on the right than the left. His alignment is pretty good at this point, but again, it will deteriorate as he grows. There are two approaches to discuss with your therapists and physicians and surgeons. The first and most common is a wait and see approach, possibly with a few Botox injections along the way. Then corrective orthopedic surgery when he is bad enough. The data reveals that this will result in a predictable loss in function.
“Insanity: doing the same thing over and over again and expecting different results.”
– Albert Einstein
The other approach is to assess what can be done to mitigate the expected loss of function. The spasticity will not magically go away as he grows. It will only get worse, magnified by body distortion. This is the time to see a good spasticity management team for an evaluation. There are best practice and evidence based interventions that work in both spasticity management and orthopedic surgery.2 Correcting the problems in early puberty makes sense…we know unattended, it will get worse.
Years ago, at the Magee Clinic, I saw a young woman from Northern Ontario who was able to walk slowly with bilateral forarm crutches. She was on her way to Vancouver, British Columbia to have a Selective Posterior Rhizotomy (SDR). I had never heard of doing this surgery so late in life, but when I examined her, I thought it was a good idea. She had had orthopedic surgery in the past and had maintained good body alignment post sugery. But she could not walk far, dress her lower body independently and fought her spastic tone daily, especially in the cold. Winters are long in Northern Ontario.
I was optimistic, but when she walked in to see me post SDR without her crutches, six weeks later, you could have knocked me over with a feather! Her tone was normal and she was stronger. She had done a really rigorous strengthening program post-operatively and it worked.
Since then, I have seen other great results of SDR. In some teenagers with GMFCS Level IV and V, a Baclofen pump has allowed more comfortable posture and function. The older the person and the higher the level of involvement, the more likely it is that orthopedic surgery will be needed as well. The alternative is functional deterioration and musculoskeletal pain. How Much Does It Hurt? Part 2
Each child is a unique individual and parents need to weigh their options carefully. I have no vested interest in a family’s choice for their child, as long as the choices are made from a base of knowledge that includes the long term results of non-action.
As ever, I look forward to your comments and questions.
- Steven E. Hanna et al. “Stability and decline in gross motor function among children and youth with cerebral palsy aged 2 to 21 years.” Developmental Medicine & Child Neurology, 51 (2009): 295-302.
- Iona Novak et al., “A systematic review of interventions for children with cerebral palsy: state of the evidence”, Developmental Medicine & Child Neurology, 55 (2013): 885-910.
READ ALSO
Will My Child Walk? Setting Age Appropriate Goals
Body Growth Increases Spasticity
Test and Test Again: Brains Keep Growing
Baby Brain Neuroplasticity
This is our exact situation. My 12 year old is getting tighter, especially in the wrist. She is three years post stroke. She has done Botox twice in the last year but the affects don’t last. The doctor mentioned surgery. The therapist thinks my daughter has hit a plateau and doesn’t really need therapy. I am beyond frustrated because I see the tightness increasing as she grows. I feel like I am hitting my head against the wall or having doors closed one after another. There are no spasticity teams where I live. Advice please. I’m desperate.
Dear Kendra, hands are difficult.I cannot advise what to do in your case, but only give suggestions of what others have found helpful. In addition to the Botox, ask your therapist about a splint to hold her wrist and hand in a good position. If she has contractures, talk to the therapist about either serial casting or other methods to straighten it out.If the main problem is the upper limb, ask to see a hand specialist…usually an OT.You may find help in a therapist who normally treats an adult with a stroke. Hope this helps.
Kendra, My name is Bob Eskew and I am a pediatric PT who has cerebral palsy including involvement in my left upper extremity. As usual, Dr. Pape had some great advice! I also cannot comment on your specific case but the following have been helpful in similar cases. I would have your therapist look at stereognosis or your daughter’s ability to identify common objects by feel alone. Another prognostic factor would be how often she uses her hand as a helper (an accelerometer worn over several days can be helpful). Electrical stimulation to the upper extremity may be helpful as well. The Bioness H200 would be something at which to look. But above all, strengthen, strengthen, strengthen! Kindest regards!
Hello!
Please could you describe what is a stregthening program. Thank you!
Strengthening programs are determined by the child’s specific needs. You should ask your physical therapist what exercises you can do at home to help things along.
Thank you for your blog posts on setting goals, pushing boundaries, and having hope. My son has triplegic cerebral palsy as the result of 3 massive strokes at birth, and is currently at a “strong” level GMFCS 4, weak GMFCS 3. I’ve always thought that he’s going to do more than some of his therapists are telling me (he is already doing SO much more than what his NICU doctors had suggested he might do) and sometimes I feel that they’ve given up on making more progress, thinking that he will never move from that GMFCS level 4. Your posts help keep me in check, help push me to do more research on possible therapies and treatments for him, and help me to keep asking questions and pushing to help our son’s brain continue to make connections. He just turned 2 and I know that there’s so much more that he can do. Thank you for all that you do!
Dear Camie, Thank you for your comment. I completely agree with you that two years old is far too early to assign a prognosis for child with cerebral palsy. If you read my book “The Boy Who Could Run But Not Walk: Understanding Neuroplasticity in the Child’s Brain” you will learn that the GMFCS level determined at age 2 frequently changes. Most children show significant improvement for 6-8 years with current treatments. In the teenage years, the long-term studies show that our regular therapy fails to create continued improvement during puberty. However, significant gains from level IV to III and higher are still possible with modern spasticity management, surgery, and a dedicated intensive program of strengthening. If you watch my TEDx talk, that can be accessed on the home page of my website, you’ll see how much change Christine was able to manage starting at age 34years. Keep up your optimism and great work for your son.