 A proportion of children with neonatal encephalopathy have damage to the brainstem nuclei and/or cerebellar damage. Depending upon the extent and site of damage, the child may have Ataxia, Athetosis or Choreoathetosis. The site(s) of brain damage in this group of movement disorders can be quite variable, but the common denominator is muscle weakness and poor proprioception. Proprioception is your awareness of where you are in space. It is the sum total of input from all sensory organs that is integrated in the brainstem and cerebellum and sent on to the cortex.
A proportion of children with neonatal encephalopathy have damage to the brainstem nuclei and/or cerebellar damage. Depending upon the extent and site of damage, the child may have Ataxia, Athetosis or Choreoathetosis. The site(s) of brain damage in this group of movement disorders can be quite variable, but the common denominator is muscle weakness and poor proprioception. Proprioception is your awareness of where you are in space. It is the sum total of input from all sensory organs that is integrated in the brainstem and cerebellum and sent on to the cortex.
This previous post (Athetosis and Choreoathetosis) describes the brain pathology and presentation of athetosis and choreoathetosis and a before and after video demonstrates the effect of improved muscle awareness and strength using low-level electrical stimulation, at night, during sleep. This infant had a major change in motor function after only 8 months of Threshold Electrical Stimulation (TES) to the trunk muscles.
In the older child, the uncontrolled movements often become even more erratic and difficult to control. Just as spasticity changes over time, the involuntary movements also increase as the child moves against gravity. They are rare under 6-12 months and some do not become obvious until 2-3 years. It is almost as if their brains are exaggerating the body movements to increase the amount of feedback. Anything that increases the core stability, giving the child more awareness, helps. In this previous post (Quick Fixes – Take Your Therapist’s Hands Home with You), you can see a dramatic change in number and severity of large athetoid movements with a TheraTogs compression garment.
Deep water jogging is another very effective intervention. When this child was first put in the water with a Wet Vest flotation device, she could only manage to stay upright for a few seconds. She gradually learned how to move in the water and discovered, for the first time, the joy of moving freely. The out of gravity experience in the water compensated for her muscle weakness. As she improved, she became stronger and developed more cardiovascular fitness. Better breath control improved her speech as well. Being immersed in the water gave her more information of where her body was in space and the added resistance of the water with movement worked like a compression vest.
All of these interventions are aimed at improving proprioceptive awareness. The results are obvious in weeks, not years, and in my opinion, well worth a trial in children with movement disorders. I would love to hear from more about your experience with any or all of these interventions.
Where To Find It
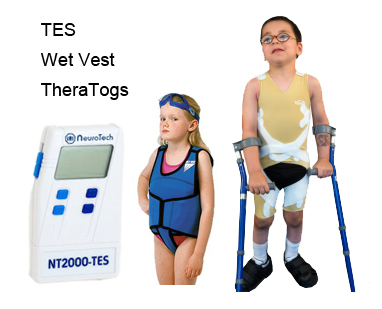
Threshold Electrical Stimulation (TES)
www.advancedmusclestimulators.com
Theratogs – Therapy You Wear
www.theratogs.com
Wet Vest II – Custom sizing is available
www.hydrofit.com
Further Reading
If you are new to this Blog and have a child with cerebral palsy, I suggest you read the current series, of which this post is number 5. It is important that parents understand the range of diagnoses and impairments in the CP spectrum to better enable you to talk with your therapists and physicians. The goal is to move towards lesion-specific therapies.
First
Too Little Too Late
Second
Do Brain Scans Improve Diagnostic Accuracy?
Third
Spastic Diplegia – Cure For Some, Improvement For All
Fourth
Hypoxic Ischemic Encephalopathy [HIE] or Neonatal Encephalopathy [NE]?
Hi Karen, I was so interested to read your article. My son has Athetoid CP and there is very little I see written about it. One therapist here in Australia told me that they don’t call it that anymore. My son has pure Athetoid CP so makes up a very small percentage of the CP population which has made it hard to learn from others as to what will or won’t work with him
We started ‘swimming lessons’ with a swimming program for children with special needs. The program became about having him move indenpendently in the water in whatever way possible. He started with pool noodles and a life vest but can now walk independently around the pool. We were thrilled with this improvement over a long period of time and found that this then translated into him walking more stably on ‘dry land’. So at the time we didn’t really know what we were doing as such but we were unknowling doing underwater jogging as you describe above. I can’t receommend this enough as our son took his first unaided steps at 18 years. This isn’t just from the work in the water of course. We continued to walk him hand on hand around the house, to the car and did other therapy in conjunction with the swimming. I think the water allows an independence that can’t be beat with the buoyancy etc.
Now if we could just crack why his sleep is so affected I’d be a very happy mother. Uninterupted sleep would be a miracle and it seems someting of a mystery to sleep specialists who usually deal with ‘regular’ kids who they can ‘fix’ in a few visits.
I really enjoyed the article. Thank you.
Julie
Hi Karen,
Thank you for this post. It is amazing to see the change that occur with something as simple as giving the child an improvement in proprioception and awareness. As a therapist it can be difficult to know where to start with a child with a movement disorder, so these interventions that you describe brings the child to a point where other more traditional therapies such as gait training, can be successfully implemented.
I recently completed an intensive for a child with a movement disorder here in our clinic. We put her in a Spio TLSO and as soon as it was on, her body quieted and she said: “Thank you – I like this”. The functional changes that then happened in the course of the week she was here were quite astonishing. Here is a link to the web page where we have video of the changes that happened as a result of the intensive: http://www.sbstherapycenter.com/#!services2/cctp. (this particular case is the last one described on the page)
Thank you for all the inspiration from your blog
Pia
Hi Karen ,
Do you recommend warm water in the pool for exercises or any regular swimming pool will solve the purpose ?
Thanks ,
Divy
Divy, it really depends on the person. Many find warm water better, but if it is not available, then there are water exercise suits that keep you warm in most pools.This is an example of the types of garments that are used.http://www.hydrofit.com/apparel/
Thank you for your question.
Hi Karen,
Thank you for your helpful posts on an array of topics regarding CP. What is your take on athetoid/mixed cp with a normal MRI?
Good question Danielle.In most children, an MRI scan will demonstrate the areas of brain damage. Failure may relate to the timing of the scan – most often done too early in the process or that the problem is caused by a more diffuse one not visible on the scan.I would discuss this with a neurologist with an interest in movement disorders.I believe an accurate diagnosis is important and a normal MRI is unusual. Hope this helps and I would like to know the outcome. Best wishes, Karen
Thank you Karen. Per the recommendation of my son’s neurologist, we waited until 2 years old to do his first MRI. When j questioned a repeat, the CP team didn’t feel it necessary. If you know of any neurologists on the east coast that specialize in motor disorders. Currently, all of the specialists are at Boston Children’s. Thank you!
An MRI at 2 years or older should reveal anatomic problems. IF your son’s scan was normal, I agree with your CP that it is not necessary.
However, seeing a neurologist who specializes in motor disorders is a separate question. In my experience, when the diagnosis is unusual or unclear, it is worth seeing a specialist.I would ask you paediatrician for help in locating the right person to see.
Hi Karen,
I want to thank you for your guidance. We had Whole Exome Sequencing which lead to the findings of a spontaneous genetic mutation of the HPRT1 gene. It presents very similarly to mixed type CP. Thank you for your input in the past.
Danielle
I just wanted to say thanks to replying my prior post and directing me to this page (it took a while for me to realize you’d replied). As a parent so much of this stuff is a mystery and it really helps that you provide so much information here.
Hi Karen,
So if I wanted to try tes on my child during sleep, how low of settings would I use?
Unfortunately, the former TES program is not available due to the manufacturers of the equipment leaving the market. Not enough demand.